Содержание
- 2. Plan of lecture: Anti-inflammatory agents Anti-allergic drugs Immunomodulators
- 3. Inflammation Inflammation is a complex protective response of the organism to injury caused by damaging agents.
- 4. Mediators of inflammation Prostaglandins Bradykinin Serotonin Histamine Interleukins-2 – 6, 10, 12,13 Platelet activating factor Gamma-Interferon
- 5. The role of some prostaglandins in the body PGE 2 – vasodilation, bronchodilation, inhibition of gastric
- 6. Cyclo-oxygenase (COX) Exists in the tissue as constitutive isoform (COX-1). At site of inflammation, cytokines stim
- 7. NSAIDs – nonsteroidal anti-inflammatory drugs
- 8. 1. Nonsteroidal anti-inflammatory drugs (NSAIDs) Nonselective COX inhibitors 1. Salicylates *Acetylsalicylic acid (Aspirin) * Salicylamide 2.
- 9. Selective COX inhibitors Preferential COX-2 inhibitors Nimesulide Meloxicam Nabumeton Selective COX-2 inhibitors Celecoxib Parecoxib Rofecoxib NB!!!These
- 10. Mechanism of action of NSAIDs (Non-Steroidal Anti-Inflammatory Drugs) • Act by inhibiting CycloOXygenases (COX) => no
- 11. Mechanism of anti-inflammatory drugs’ action
- 12. Pharmacological effects of NSAIDs Anti-inflammatory Analgesic Antipyretic Antiplatelet (Aspirin) Closure of ductus arteriosus in newborn
- 13. Clinical uses of NSAIDs 1. Pain: headache, toothache, myalgia, backpain; 2. Fever; 3. Arthritises: rheumatiod arthritis,
- 15. Side effects of NSAIDs 1. GIT disturbances: epigastric pain, nausea, gastric peptic ulcer (especially aspirin), gastrointestinal
- 16. Contraindications A) Pregnancy B) Haemophilic patients C) Hypersensitivity reactions D) Viral infections mainly in children E)
- 17. Drugs interaction Potentiates the gastric irritant effect of alcohol Potentiates the hypoglycaemic effects of oral hypoglycaemic
- 18. The Salicylates - ASPIRIN Duration of action ~ 4 hr. Orally taken. Weak acid (pKa ~
- 19. ASPIRIN - Therapeutic Uses Antipyretic, analgesic. Anti-inflammatory: rheumatic fever, rheumatoid arthritis (joint dis), other rheumatological diseases.
- 20. Propionic acid derivatives IBUPROFEN: Pharmacokinetics Rapidly absorbed after oral ingestion. Half-life 1-2 hours Highly bound to
- 21. IBUPROFEN The same mechanism & pharmacological actions of aspirin Except that it is reversible inhibitor for
- 22. Clinical uses A) Analgesic B) Antipyretic C) Anti-inflammatory D)Acute gouty arthritis E) Patent ductus arteriosus
- 23. Preparations of Ibuprofen Oral preparations. Topical cream for osteoarthritis. A liquid gel for rapid relief of
- 24. Adverse effects 1.Gastric upset (less frequent than aspirin). 2.Fluid retention 3.Hypersensetivity reactions 4.Ocular disturbances 5.Rare hematologic
- 25. Contraindications 1. Peptic ulcer 2. Allergic patients to aspirin 3. Kidney impairment 4.Liver diseases 5.Pregnancy 6.Haemophilic
- 26. Piroxicam Mechanism of actions: A) Non-selective inhibitors to COX1 & COX2 B) Traps free radicals C)
- 27. Pharmacokinetics Well absorbed orally Half- Life 45 hours Given once daily
- 28. Adverse effects Less frequent gastric upset (20%). Dizziness. Tinnitus. Headache. Allergy.
- 29. Acetic acid derivatives DICLOFENAC Mechanism of action Non-selective inhibitor to COX1 & COX2. More potent as
- 30. Clinical uses DICLOFENAC A) Any inflammatory conditions B) Musculoskeletal pain C) Dysmenorrhoea D)Acute gouty arthritis E)
- 31. Adverse effects DICLOFENAC Gastric upset Renal impairment Elevation of serum aminotransferase Salt & water retention
- 32. Preparations of DICLOFENAC Diclofenac with misoprostol decreases upper gastrointestinal ulceration, but result in diarrhea. Diclofenac with
- 33. Selective COX 2 inhibitors Advantages: 1. Highly selective inhibitors to COX2 enzyme. 2. Potent anti-inflammatory. 3.
- 34. Selective Cox 2 inhibitors 5. Lower incidence of gastric upset. 6. No effect on platelet aggregation
- 35. Selective Cox 2 inhibitors 9- They are recommended in postoperative patients undergoing bone repair. 10- Also,
- 36. SAIDs – steroidal anti-inflammatory drugs
- 37. Steroidal anti-inflammatory drugs 1. Short-acting glucocorticoids (natural) Hydrocortisone Cortisone 2. Intermediate-acting glucocorticoids Prednisone Prednisolone Methylprednisolone Triamcinolone
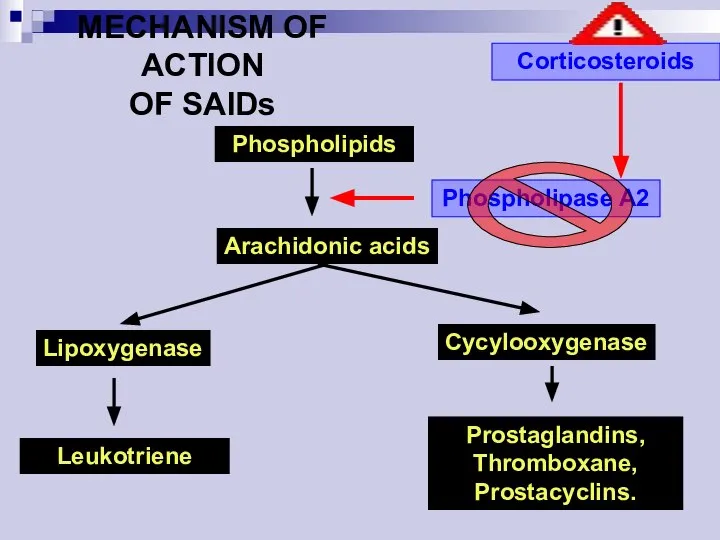
- 40. Phospholipids Arachidonic acids Lipoxygenase Cycylooxygenase Leukotriene Prostaglandins, Thromboxane, Prostacyclins. Phospholipase A2 Corticosteroids MECHANISM OF ACTION OF
- 41. Clinical uses of SAIDs Adrenal insufficiency Arthrities Collagen diseases (systemic lupus erhymatosis, scleroderma) Bronchial asthma Severe
- 42. Main side effects of SAIDs Susceptibility to infections Delayed healing of wounds Osteoporosis Growth retardation in
- 43. ANTI-ALLERGIC DRUGS
- 44. Allergy An allergy is a hypersensitivity disorder of the immune system. Allergic reactions occur when a
- 45. mild/cutaneous mild to moderate severe/ anaphylactic erythema, urticaria, and/or itching skin reactions, tachycardia, dysrhythmias, moderate hypotension,
- 46. Histamine exerts its effects on many tissues and organs: It is not a drug but is
- 47. Pathophysiological Actions of Histamine Cellular mediator of immediate hypersensitivity reaction and acute inflammatory response Anaphylaxis Seasonal
- 48. Pharmacological Effects of Histamine Ranges from mild allergic symptoms to anaphylactic shock Involves both the H1
- 49. (Oedema of Quincke, Stevence-Johnson syndrome)
- 53. Antiallergic drugs 1. Antihistaminics 2. Corticosteroids 3. Mast cell stabilisers 4.Antileukotriene drugs
- 54. histaglobulin
- 58. Histamine-related Drugs Mast Cell Stabilizers (Cromolyn Na, Nedocromil –Tilade -, Albuterol) H1 Receptor Antagonists (1st and
- 59. First Generation ANTIHISTAMINE Agents Ethanolamines: DIPHENHYDRAMINE (Benadryl) CLEMASTINE (Tavist) Ethylenediamine:TRIPELENNAMINE Alkylamine:CHLORPHENIRAMINE (Chlortrimeton) Phenothiazine:PROMETHAZINE (Phenergan) Piperazines: HYDROXYZINE
- 60. Uses: Adjunctive in anaphylaxis and other cases where histamine release can occur (H2 antagonist, and epinephrine
- 61. First Generation Agents Adverse Effects: Sedation (Paradoxical Excitation in children) Dizziness Fatigue Tachydysrhythmias in overdose -
- 62. Drug interactions: Additive with classical antimuscarinics Potentiate CNS depressants opioids sedatives general and narcotic analgesics alcohol
- 63. Uses Antiallergy Examples CETIRIZINE (ZYRTEC) FEXOFENADINE (ALLEGRA) LORATADINE (CLARITIN) DESLORATADINE (CLARINEX- FDA APPROVED IN 2002) LORATADINE
- 65. Histamine H1- Antagonists First Generation: !!!Sedating!!! Second Generation: !!!Non sedating!!!
- 66. Advantages of 2nd generation antihistaminics Higher H1 selectivity, absence of anticholinergic side effects Absence of inhibitory
- 67. Mast cell stabilisers Cromolyn sodium (Sodium cromoglycate) Nedocromil sodium Ketotifen Corticosteroids (vide supra)
- 69. Antileukotriene drugs Montelukast Zafirlukast Mechanism: competitive block of LT1 receptors Clinical use: bronchial asthma
- 71. Immunomodulators
- 83. Скачать презентацию















































































 Проблемы и перспективы современной медицины: философский анализ
Проблемы и перспективы современной медицины: философский анализ Нарушения слуха
Нарушения слуха Сестринская помощь при воздушно-капельных инфекциях. Риновирусная инфекция
Сестринская помощь при воздушно-капельных инфекциях. Риновирусная инфекция Керамические виниры
Керамические виниры Тістің тіс жегі емес ақауларын нактамалау
Тістің тіс жегі емес ақауларын нактамалау Лечение пульпитов временных и постоянных зубов. Особенности эндодонтического лечения пульпитов у детей
Лечение пульпитов временных и постоянных зубов. Особенности эндодонтического лечения пульпитов у детей Классификация психопатий
Классификация психопатий Влияние игр на человека
Влияние игр на человека Егде және қарт жастағы (геронтологиялық аспект)адамдарының психосоматикалық бұзылыстары
Егде және қарт жастағы (геронтологиялық аспект)адамдарының психосоматикалық бұзылыстары Чем вредны памперсы
Чем вредны памперсы Роль прокоагулянтов, антикоагулянтов и факторов фибринолиза слюны
Роль прокоагулянтов, антикоагулянтов и факторов фибринолиза слюны Психолого-педагогическая характеристика детей с задержкой психического развития
Психолого-педагогическая характеристика детей с задержкой психического развития Клинико-лабораторные особенности менингитов у детей раннего возраста
Клинико-лабораторные особенности менингитов у детей раннего возраста Профилактика ОРВИ, гриппа и коронавирусной инфекции. Для учащихся 5-11 классов
Профилактика ОРВИ, гриппа и коронавирусной инфекции. Для учащихся 5-11 классов Методи електролікування
Методи електролікування Рак предстательной железы
Рак предстательной железы Электрожарақаттар
Электрожарақаттар Потовые железы. Ориентировочная реакция и привыкание
Потовые железы. Ориентировочная реакция и привыкание Микробиология дифтерии
Микробиология дифтерии Декларация целей и задач «ГУЗ Старосахчинская участковая больница» на 2019 год
Декларация целей и задач «ГУЗ Старосахчинская участковая больница» на 2019 год Пороки развития гортани
Пороки развития гортани Физиология сердечно-сосудистой системы
Физиология сердечно-сосудистой системы Предмет і місце педіатрії в системі охорони здоров`я. Періоди дитячого віку. Особливості періоду новонародженості
Предмет і місце педіатрії в системі охорони здоров`я. Періоди дитячого віку. Особливості періоду новонародженості Внутриличностные конфликты
Внутриличностные конфликты Электролечение постоянным и импульсным током низкой частоты
Электролечение постоянным и импульсным током низкой частоты Роль акушерки в профилактике геморрагического шока в послеродовом периоде
Роль акушерки в профилактике геморрагического шока в послеродовом периоде Роль среднего медицинского персонала в проекте Бережливая поликлиника
Роль среднего медицинского персонала в проекте Бережливая поликлиника Муниципальное автономное учреждение Реабилитационно - оздоровительный центр
Муниципальное автономное учреждение Реабилитационно - оздоровительный центр