Содержание
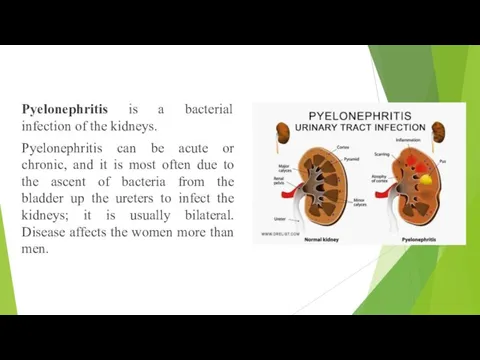
- 2. Pyelonephritis is a bacterial infection of the kidneys. Pyelonephritis can be acute or chronic, and it
- 3. Incidence: About 3 to 7 out of 10,000 people. Predisposing factors: Obstruction of the urinary tract
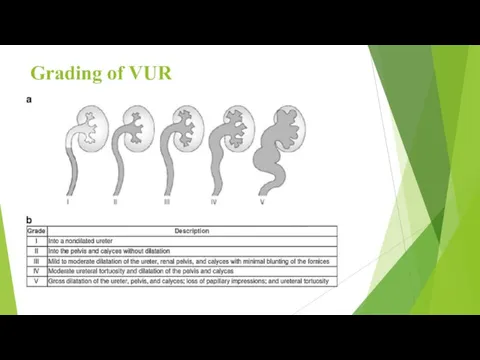
- 4. Grading of VUR
- 5. Causative organisms: Gram negative organism: E.coli (common), Proteus mirabilis, Citrobacter, klebsiella, enterobacter, proteus pseudomonas aeruginosa; Gram
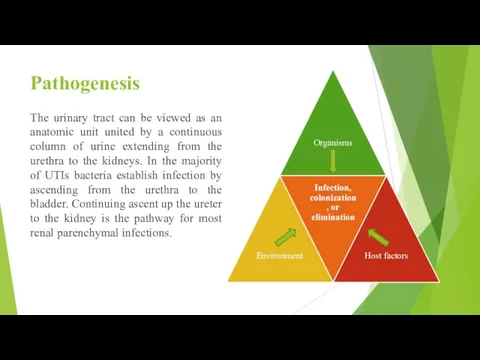
- 6. Pathogenesis The urinary tract can be viewed as an anatomic unit united by a continuous column
- 8. Signs and symptoms Signs and symptoms of a kidney infection might include: Fever Chills Back, side
- 9. Acute pyelonephritis Acute pyelonephritis is an exudative purulent localized inflammation of the renal pelvis (collecting system)
- 10. Chronic pyelonephritis Chronic pyelonephritis implies recurrent kidney infections and can result in scarring of the renal
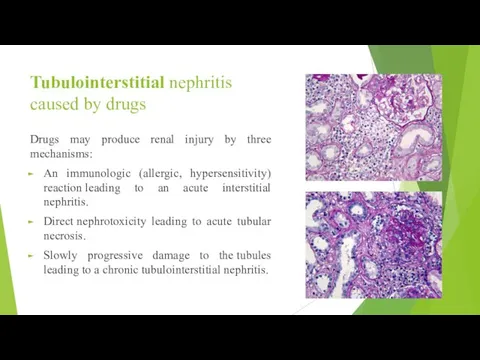
- 12. Tubulointerstitial nephritis caused by drugs Drugs may produce renal injury by three mechanisms: An immunologic (allergic,
- 13. Acute drug induced tubulointerstitial nephritis may be induced by synthetic penicillins (methicillin, ampicillin), sulfonamides, rifampin, diuretics
- 14. Diagnostics Physical examination: - soreness in palpation in the area of the projection of the kidneys;
- 15. Imaging studies If a kidney stone is suspected (e.g. on the basis of characteristic colicky pain
- 16. Purpose of treatment: consists in elimination of infectious and inflammatory process, possible only at restoration of
- 17. Detoxification therapy: plentiful drink; parenteral infusion therapy in the form of solutions of glucose 5-10% and
- 18. The list of basic medicines: 1. Amoxicillin + clavulanic acid, coated tablets 250 mg / 125
- 20. Скачать презентацию
Pyelonephritis is a bacterial infection of the kidneys.
Pyelonephritis can be
Pyelonephritis is a bacterial infection of the kidneys.
Pyelonephritis can be
Incidence:
About 3 to 7 out of 10,000 people.
Predisposing factors:
Obstruction of the
Incidence:
About 3 to 7 out of 10,000 people.
Predisposing factors:
Obstruction of the
Female: Shorter urethra
Male : uncircumcised infant bacterial colonization inside prepuce and urethra
Vesicoureteric reflux: Normally, the urine does not ascend along the ureters during micturition due to the oblique course of the intravesical portion of the ureter, which provide asphincter-like effect during contraction of the bladder.) If this effect is disturbed due to congenital or acquired reasons, the urine will ascend along the ureter and may even reach the kidneys during bladder emptying.
Bilharsisis
Instrumentation of the urinary tract.
Diabetes mellitus
Female more due to short urethra.
Pregnancy due to hormonal relaxation of smooth muscle and pressure of the gravid uterus
Grading of VUR
Grading of VUR
Causative organisms:
Gram negative organism: E.coli (common), Proteus mirabilis, Citrobacter, klebsiella,
Causative organisms:
Gram negative organism: E.coli (common), Proteus mirabilis, Citrobacter, klebsiella,
Gram positive organism, Staph.saprophyticus, Staph.epidermidis enterococcus, Corynebacteria and lactobacilli.
Routes of infection:
Ascending infection from the lower urinary tract.
Lymphatic spread from the intestinal tract.
Blood borne infection complicating boils or carbuncles.
Pathology:
Acute pyelonephritis
Chronic pyelonephritis
Pathogenesis
The urinary tract can be viewed as an anatomic unit united
Pathogenesis
The urinary tract can be viewed as an anatomic unit united
Signs and symptoms
Signs and symptoms of a kidney infection might include:
Fever
Chills
Back,
Signs and symptoms
Signs and symptoms of a kidney infection might include:
Fever
Chills
Back,
Abdominal pain
Frequent urination
Strong, persistent urge to urinate
Burning sensation or pain when urinating
Nausea and vomiting
Pus or blood in your urine (hematuria)
Urine that smells bad or is cloudy
Acute pyelonephritis
Acute pyelonephritis is an exudative purulent localized inflammation of the renal
Acute pyelonephritis
Acute pyelonephritis is an exudative purulent localized inflammation of the renal
The kidney parenchyma presents in the interstitium abscesses (suppurative necrosis), consisting in purulent exudate (pus): neutrophils, fibrin, cell debris and central germ colonies (hematoxylinophils). Tubules are damaged by exudate and may contain neutrophil casts. In the early stages, the glomerulus and vessels are normal. Gross pathology often reveals pathognomonic radiations of bleeding and suppuration through the renal pelvis to the renal cortex.
Chronic pyelonephritis
Chronic pyelonephritis implies recurrent kidney infections and can result in scarring of
Chronic pyelonephritis
Chronic pyelonephritis implies recurrent kidney infections and can result in scarring of
Chronic pyelonephritis with reduced kidney size and focal cortical thinning. Measurement of kidney length on the US image is illustrated by ‘+’ and a dashed line.
Tubulointerstitial nephritis caused by drugs
Drugs may produce renal injury by three
Tubulointerstitial nephritis caused by drugs
Drugs may produce renal injury by three
An immunologic (allergic, hypersensitivity) reaction leading to an acute interstitial nephritis.
Direct nephrotoxicity leading to acute tubular necrosis.
Slowly progressive damage to the tubules leading to a chronic tubulointerstitial nephritis.
Acute drug induced tubulointerstitial nephritis may be induced by synthetic penicillins
Acute drug induced tubulointerstitial nephritis may be induced by synthetic penicillins
Acute tubular necrosis, due to direct nephrotoxicity may be induced by antibiotics (gentamicin) and antifungal agents (amphotericin B). It leads to acute renal failure.
Chronic tubulointerstitial nephritis may be induced by heavy usage of analgesic, mainly those containing phenacetin (analgesic nephropathy). It may end in chronic renal failure.
Diagnostics
Physical examination:
- soreness in palpation in the area of the projection
Diagnostics
Physical examination:
- soreness in palpation in the area of the projection
- arterial hypertension.
Laboratory research:
- bacteriuria 105;
- leukocyturia;
- erythrocyturia;
- proteinuria (β2-microglobulin);
- reduction of the concentration function;
- GFR;
- anemia
Imaging studies
If a kidney stone is suspected (e.g. on the basis
Imaging studies
If a kidney stone is suspected (e.g. on the basis
Ultrasound findings that indicate pyelonephritis are enlargement of the kidney, edema in the renal sinus or parenchyma, bleeding, loss of corticomedullary differentiation, abscess formation, or an areas of poor blood flow on doppler ultrasound. However, ultrasound findings are seen in only 20% to 24% of people with pyelonephritis.
A DMSA scan is a radionuclide scan that uses dimercaptosuccinic acid in assessing the kidney morphology. It is now the most reliable test for the diagnosis of acute pyelonephritis.
Purpose of treatment: consists in elimination of infectious and inflammatory process,
Purpose of treatment: consists in elimination of infectious and inflammatory process,
Indications for hospitalization: In acute secondary pyelonephritis, urgent hospitalization is necessary in the urological department in connection with the possible need for an urgent open surgery to prevent severe, life-threatening complications (toxic shock). In acute primary pyelonephritis, hospitalization is also desirable, since a concealed violation is possible outflow of urine. In addition, with this form of the disease, the serous phase can quickly progress to purulent, requiring urgent surgical treatment. In extreme cases, with confidence in the diagnosis of acute primary pyelonephritis, antibiotic therapy can also be started on an outpatient basis.
Unambiguously patients need the emergency hospitalization:
▪ with acute pyelonephritis of a single or only functioning kidney;
▪ exacerbation of chronic pyelonephritis and signs of renal insufficiency;
▪ acute pyelonephritis on the background of diabetes mellitus or immunodeficiency;
▪ suspected purulent process in the kidney;
▪ acute pyelonephritis with ineffective antibiotic therapy.
Detoxification therapy:
plentiful drink;
parenteral infusion therapy in the form of solutions of
Detoxification therapy:
plentiful drink;
parenteral infusion therapy in the form of solutions of
Antibiotic therapy: The basic principle is the early and long-term appointment of antimicrobial agents in strict accordance with the sensitivity to them microflora inoculated from the urine, the alternation of antimicrobials or their combined use.
1. Gram-positive: semi-synthetic penicillins (ampicillin, amoxicillin + clavulanic acid).
2. Gram-negative: co-trimoxazole + fluoroquine (ciprofloxacin, ofloxacin, norfloxacin).
3. Nosocomial infection: aminoglycosides (gentamicin) + cephalosporins (ceftriaxone, cefotaxime, ceftazidime).
4. Reserve antibiotics: imipenem, amikacin.
5. Uroantiseptics: nitrofurans (furagin).
The duration of antibiotic therapy is determined by the severity of the infection process, the presence of complications.
In some cases, supportive therapy with other antibacterial agents - uroseptics (furagin 1-2 mg / kg / night, co-trimoxazole - 120-240 mg per night) is necessary.
In parallel, it is necessary to carry out antifungal therapy (itraconazole), correction of intestinal microflora, immunostimulant therapy.
The list of basic medicines:
1. Amoxicillin + clavulanic acid, coated tablets
The list of basic medicines:
1. Amoxicillin + clavulanic acid, coated tablets
2. Ampicillin - 500 mg, fl.
3. Ceftriaxone 500 mg, 1 g, fl.
4. Imipenems
5. Fluoroquine (ciprofloxacin, ofloxacin, norfloxacin)
6. Co-trimoxazole - 120 mg, 480 mg, tab.
7. Cefuroxime axetil - 125 mg, 250 mg, tablets, suspensions
8. Gentamicin 40 mg, 80 mg, fl.
9. Furagin 50 mg, tab.
10. Enalapril 5 mg, 10 mg, tab.













 Курс Родить легко
Курс Родить легко Челюстно-лицевая ортопедия. Цель, задачи. Классификация переломов челюстей. Причины и механизм смещения отломков. (Тема 3)
Челюстно-лицевая ортопедия. Цель, задачи. Классификация переломов челюстей. Причины и механизм смещения отломков. (Тема 3) Болезни новорождённых
Болезни новорождённых Суррогатное материнство
Суррогатное материнство Переноска, транспортировка раненых и пострадавших
Переноска, транспортировка раненых и пострадавших Анафилактический шок. Неотложная помощь, интенсивная терапия
Анафилактический шок. Неотложная помощь, интенсивная терапия Системная красная волчанка
Системная красная волчанка Ишемическая болезнь сердца
Ишемическая болезнь сердца Техническое обеспечение современной анестезии
Техническое обеспечение современной анестезии Внебольничная пневмония
Внебольничная пневмония Бронзовая болезнь или Болезнь Аддисона
Бронзовая болезнь или Болезнь Аддисона Информация для медицинских и фармацевтических работников CP-266252
Информация для медицинских и фармацевтических работников CP-266252 Ауыз қуысының шырышты қабатының созылмалы аурулары. Ортопедиялық емдеу тәсілдер
Ауыз қуысының шырышты қабатының созылмалы аурулары. Ортопедиялық емдеу тәсілдер Деформирующий остеоартроз. Причины, симптомы, диагностика и лечение
Деформирующий остеоартроз. Причины, симптомы, диагностика и лечение Гигиена зубов и полости рта. Гигиена тела и кожи
Гигиена зубов и полости рта. Гигиена тела и кожи Психология или психиатрия?
Психология или психиатрия? ЕГИСЗ. Федеральный регистр лиц, больных туберкулезом. Правила учета сведений для расчета основных показателей
ЕГИСЗ. Федеральный регистр лиц, больных туберкулезом. Правила учета сведений для расчета основных показателей Zacházení s lékařskými předpisy
Zacházení s lékařskými předpisy Нормативно-правовые основы профессиональной деятельности младшего медицинского персонала
Нормативно-правовые основы профессиональной деятельности младшего медицинского персонала Типы темперамента
Типы темперамента Лекарственные средства, влияющие на адренергические синапсы
Лекарственные средства, влияющие на адренергические синапсы Гуморальный иммунитет. Иммуноглобулины. Роль антител. Реакция антиген-антитело. (Лекция 12)
Гуморальный иммунитет. Иммуноглобулины. Роль антител. Реакция антиген-антитело. (Лекция 12) Предмет, задачи, особенности анатомии, физиологии, гигиены как науки. Основные закономерности роста и развития организма
Предмет, задачи, особенности анатомии, физиологии, гигиены как науки. Основные закономерности роста и развития организма Взаимосвязь различных факторов риска с патологией ЦНС у детей первого года жизни
Взаимосвязь различных факторов риска с патологией ЦНС у детей первого года жизни Гемотрансфузионный шок
Гемотрансфузионный шок Иммунотропные, противоаллергические и противовоспалительные средства
Иммунотропные, противоаллергические и противовоспалительные средства Нақты қылмыстар себептерінің әлеуметтік және биологиялық факторлары Әлеуметтік және биологиялық факторлардың ара қатынасы
Нақты қылмыстар себептерінің әлеуметтік және биологиялық факторлары Әлеуметтік және биологиялық факторлардың ара қатынасы Педагогічна цінність використання ігор на практичних заняттях
Педагогічна цінність використання ігор на практичних заняттях