Слайд 11

JAMA Pediatr. 2017 Aug 7;171(8):e171333. doi: 10.1001/jamapediatrics.2017.1333. Epub 2017 Aug 7.
Effect of Nebulized Hypertonic Saline Treatment in Emergency Departments on the Hospitalization Rate for Acute Bronchiolitis:
A Randomized Clinical Trial.
Angoulvant F1,2, Bellêttre X3, Milcent K4,5, Teglas JP5, Claudet I6, Le Guen CG7, de Pontual L8, Minodier P9, Dubos F10, Brouard J11, Soussan-Banini V12, Degas-Bussiere V13, Gatin A14, Schweitzer C14, Epaud R15, Ryckewaert A16, Cros P17, Marot Y18, Flahaut P19, Saunier P20, Babe P21, Patteau G1, Delebarre M10, Titomanlio L3, Vrignaud B7, Trieu TV8, Tahir A22, Regnard D23, Micheau P6, Charara O24, Henry S25, Ploin D26,27, Panjo H5, Vabret A11, Bouyer J5, Gajdos V4,5; Efficacy of 3% Hypertonic Saline in Acute Viral Bronchiolitis (GUERANDE) Study Group.
IMPORTANCE: Acute bronchiolitis is the leading cause of hospitalization among infants. Previous studies, underpowered to examine hospital admission, have found a limited benefit of nebulized hypertonic saline (HS) treatment in the pediatric emergency department (ED).
OBJECTIVE: To examine whether HS nebulization treatment would decrease the hospital admission rate among infants with a first episode of acute bronchiolitis.
DESIGN, SETTING, AND PARTICIPANTS: The Efficacy of 3% Hypertonic Saline in Acute Viral Bronchiolitis (GUERANDE) study was a multicenter, double-blind randomized clinical trial on 2 parallel groups conducted during 2 bronchiolitis seasons (October through March) from October 15, 2012, through April 15, 2014, at 24 French pediatric EDs. Among the 2445 infants (6 weeks to 12 months of age) assessed for inclusion, 777 with a first episode of acute bronchiolitis with respiratory distress and no chronic medical condition were included.
INTERVENTIONS: Two 20-minute nebulization treatments of 4 mL of HS, 3%, or 4 mL of normal saline (NS), 0.9%, given 20 minutes apart.
MAIN OUTCOMES AND MEASURES: Hospital admission rate in the 24 hours after enrollment.
RESULTS: Of the 777 infants included in the study (median age, 3 months; interquartile range, 2-5 months; 468 [60.2%] male), 385 (49.5%) were randomized to the HS group and 387 (49.8%) to the NS group (5 patients did not receive treatment). By 24 hours, 185 of 385 infants (48.1%) in the HS group were admitted compared with 202 of 387 infants (52.2%) in the NS group. The risk difference for hospitalizations was not significant according to the mixed-effects regression model (adjusted risk difference, -3.2%; 95% CI, -8.7% to 2.2%; P = .25). The mean (SD) Respiratory Distress Assessment Instrument score improvement was greater in the HS group (-3.1 [3.2]) than in the NS group (-2.4 [3.3]) (adjusted difference, -0.7; 95% CI, -1.2 to -0.2; P = .006) and similarly for the Respiratory Assessment Change Score. Mild adverse events, such as worsening of cough, occurred more frequently among children in the HS group (35 of 392 [8.9%]) than among those in the NS group (15 of 384 [3.9%]) (risk difference, 5.0%; 95% CI, 1.6%-8.4%; P = .005), with no serious adverse events.
CONCLUSIONS AND RELEVANCE: Nebulized HS treatment did not significantly reduce the rate of hospital admissions among infants with a first episode of acute moderate to severe bronchiolitis who were admitted to the pediatric ED relative to NS, but mild adverse events were more frequent in the HS group.















 День осведомленности о мышечной дистрофии Дюшенна
День осведомленности о мышечной дистрофии Дюшенна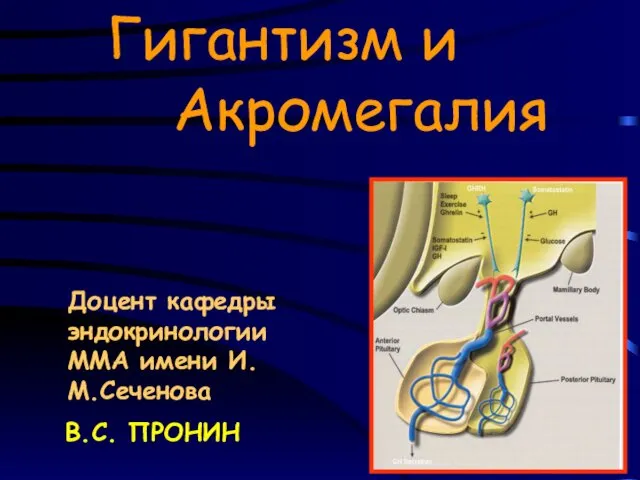 Гигантизм и акромегалия
Гигантизм и акромегалия Основы медицинской протозоологии
Основы медицинской протозоологии To study the effect of various tranquilizers and sedatives on motor co-ordination by Rota Rod test in rodents. (Lab. 3)
To study the effect of various tranquilizers and sedatives on motor co-ordination by Rota Rod test in rodents. (Lab. 3) Тромбоз мезентериальных сосудов
Тромбоз мезентериальных сосудов Основные виды и методы профилактики зависимости
Основные виды и методы профилактики зависимости Қантамырлардың жүйкелік реттелуінің бұзылысы
Қантамырлардың жүйкелік реттелуінің бұзылысы Состояние функции почек у больных с острой декомпенсацией хронической сердечной недостаточности
Состояние функции почек у больных с острой декомпенсацией хронической сердечной недостаточности Визуальная диагностика поджелудочной железы
Визуальная диагностика поджелудочной железы Витамин С в медицине
Витамин С в медицине Миниинвазивные вмешательства в кардио- и ангиохирургии
Миниинвазивные вмешательства в кардио- и ангиохирургии Мектеп жасындағы балалардың күнтізбелік тәртібі. Алты жастағы балаларды оқытуды гигиеналық ұйымдастыру қағидалары. (Дәріс 13)
Мектеп жасындағы балалардың күнтізбелік тәртібі. Алты жастағы балаларды оқытуды гигиеналық ұйымдастыру қағидалары. (Дәріс 13) Организация проведения научных исследований в медицине. Концепция развития медицинской науки до 2020 года в РК
Организация проведения научных исследований в медицине. Концепция развития медицинской науки до 2020 года в РК Геморрагические диатезы
Геморрагические диатезы Спирография
Спирография Трахеостомия
Трахеостомия Лекарственные растения. Викторина
Лекарственные растения. Викторина Диагностика СКВ
Диагностика СКВ Внутриутробная инфекция плода и новорожденного
Внутриутробная инфекция плода и новорожденного Патология щитовидной железы
Патология щитовидной железы Роль преаналитического этапа в лабораторных исследованиях. Часть 1
Роль преаналитического этапа в лабораторных исследованиях. Часть 1 Дыхательная гимнастика
Дыхательная гимнастика Чувства и эмоции
Чувства и эмоции Препараты. Карнитина хлорид
Препараты. Карнитина хлорид Моральный статус эмбриона. Моральные проблемы контрацепции. Этические проблемы вспомогательных репродуктивных технологий (ВРТ)
Моральный статус эмбриона. Моральные проблемы контрацепции. Этические проблемы вспомогательных репродуктивных технологий (ВРТ) Адаптация детей
Адаптация детей Нейродегенеративные заболевания
Нейродегенеративные заболевания Орталық жүйке жүйесінің ноцецептивтік жүйесі. Неврологиядағы ауырсыну синдромы
Орталық жүйке жүйесінің ноцецептивтік жүйесі. Неврологиядағы ауырсыну синдромы