Содержание
- 2. Medical helminthology is concerned with the study of helminthes or parasitic worms. Helminthes are trophoblastic metazoa
- 3. Transmission of helmintes: The sources of the parasites are different. Exposure of humans to the parasites
- 4. MEDICALLY IMPORTANT TREMATODES (FLUKES) 1. BLOOD FLUKES
- 5. Schistosomiasis. Shistosoma spp. It is estimated that about 600 million people in 79 countries suffer from
- 6. Definitive host: man, Intermediate host: freshwater snail Infective stage: cercariae (larvae) cercaria Adult male and female
- 7. Morphology Schistosoma mansoni. Habitat - This species lives in the veins of the intestine. Geographical distribution:
- 9. Symptoms Patients infected with S. haematobium suffer from terminal haematuria and painful micturition. There is inflammation
- 10. Diagnosis S. mansoni: ♦ Microscopic examination of the stool for eggs after concentration by sedimentation method.
- 11. Treatment Praziquantel: single oral dose of 40 mg/kg divided into two doses. Metriphonate 7.5 mg/kg. weekly
- 12. 2. LIVER FLUKES
- 13. Clonorchiasis. Clonorchis sinensis Morphology. Chinese liver fluke - adult worms live in bile ducts. Adult worm.
- 14. Symptoms: The migration of the larva up the bile duct induces desquamation, followed by hyperplasia, and
- 15. Definitive host: Humans are the principal definitive host, but dogs and other fish-eating canines act as
- 16. Treatment: Drug of choice is Praziquantel 25 mg/kg, 3 doses in 1 day. Surgical intervention may
- 17. Adults of Opisthorchis spp. are similar to, but often smaller than, Clonorchis sinensis. Adults measure approximately
- 19. Diagnosis: Microscopic identification of eggs in stool specimens. The adult fluke can also be recovered at
- 20. Diagnosis: stool examinations Imaging (ultrasound, CT, MRI). Serologic testing Treatment: Praziquantel, adults, 75mg/kg/day orally, three doses
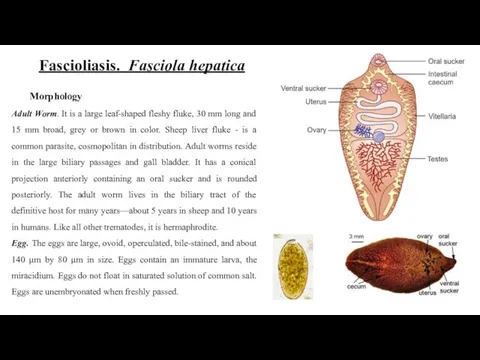
- 21. Fascioliasis. Fasciola hepatica Morphology Adult Worm. It is a large leaf-shaped fleshy fluke, 30 mm long
- 22. Symptoms: In traversing the liver tissue, it causes parenchymal injury. As humans are not its primary
- 23. Diagnosis: Stool Microscopy Blood Picture Serodiagnosis Imaging (USG, CT scan, Endoscopic Retrograde Choangiopancreatography (ERCP) and percutaneous
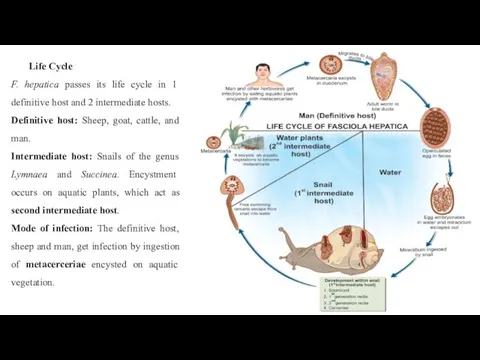
- 24. Life Cycle F. hepatica passes its life cycle in 1 definitive host and 2 intermediate hosts.
- 26. Скачать презентацию
Medical helminthology is concerned with the study of helminthes or parasitic
Medical helminthology is concerned with the study of helminthes or parasitic
Helminthes are trophoblastic metazoa (multi-cellular organisms).
Helminthes are among the common parasitic causes of human suffering. They are the cause of high morbidity and mortality of people worldwide. They cause different diseases in humans, but few helminthic infections cause life- threatening diseases. They cause anemia and malnutrition. In children they cause a reduction in academic performance. Helminthes also cause economic loss as a result of infections of domestic animals.
There is age dependent distribution of infections from geohelminthes and schistosomes. As a result of predisposing behavioral and immunological status, children disproportionately carry the burden of schistosomes and geo-helminthes.
Transmission of helmintes:
The sources of the parasites are different. Exposure of
Transmission of helmintes:
The sources of the parasites are different. Exposure of
1. Contaminated soil (Geo-helminthes), water (cercariae of blood flukes) and food (Taenia in raw meat).
2. Blood sucking insects or arthropods (as in filarial worms).
3. Domestic or wild animals harboring the parasite (as in echinococcus in dogs).
4. Person to person (as in Enterobius vermicularis, Hymenolopis nana).
5. Oneself (auto-infection) as in Enterobius vermicularis.
They enter the body through different routes including: mouth, skin and the respiratory tract by means of inhalation of airborne eggs. The Trematodes and Cestodes are groups of flat worms.
MEDICALLY IMPORTANT
TREMATODES (FLUKES)
1. BLOOD FLUKES
MEDICALLY IMPORTANT
TREMATODES (FLUKES)
1. BLOOD FLUKES
Schistosomiasis. Shistosoma spp.
It is estimated that about 600 million people in
Schistosomiasis. Shistosoma spp.
It is estimated that about 600 million people in
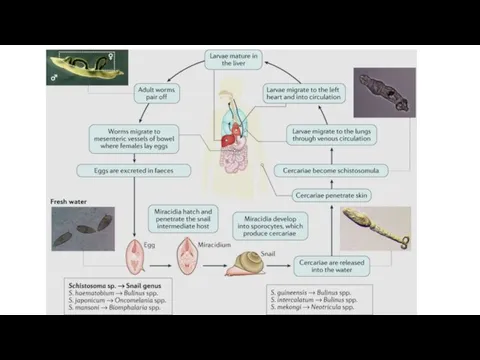
There are five medically important species:
1. Schistosoma mansoni: causes intestinal schistosomiasis.
2. Schistosoma haematobium: causes vesical (urinary) schistosomiasis.
3. Schistosoma japonicum: causes intestinal schistosomiasis.
4. Schistosoma intercalatum: causes intestinal schistosomiasis.
5. Schistosoma mekongi: causes intestinal schistosomiasis. This seems to cause milder disease in man. It causes disease in other vertebrate hosts. The first two schistosomes (S. mansoni and S. haematobium) are prevalent in Ethiopia.
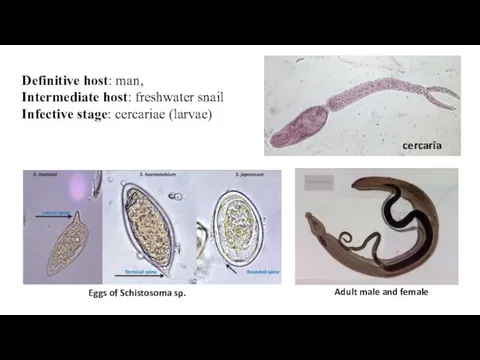
Definitive host: man,
Intermediate host: freshwater snail
Infective stage: cercariae (larvae)
cercaria
Adult male and
Definitive host: man,
Intermediate host: freshwater snail
Infective stage: cercariae (larvae)
cercaria
Adult male and
Eggs of Schistosoma sp.
Morphology
Schistosoma mansoni. Habitat - This species lives in the veins of
Morphology
Schistosoma mansoni. Habitat - This species lives in the veins of
Schistosoma haematobium. Etiology - urinary Scistosomiasis. Habitat - The worm lives in the veins of the bladder of humans. The peak prevalence is the 10-14 year age group. The snail hosts that harbor S. haematobium are the genera Bulinus and Physopsis. Male: The male ranges in size from 1-1.5 cm in length. The body is covered by fine tubercles. It has 4-5 testes. Female: The female ranges in size from 2-2.5 cm in length. The ovary is present in the posterior third. Vitelline glands occupy the posterior thirds. Uterus is long containing many ova. It lays about 20-200 eggs daily. Distribution: In Ethiopia, S. haematobium is found in the Lower Awash Valley in the east and in Benshangul-Gumuz (Assossa) regional state in the west in low altitudes below 1000 meters above sea level.
Schistosoma japonicum. The female adult worm lays about 500-3500 eggs daily. The eggs are ovoid, bearing only a minute lateral spine or a small knob postero-laterally. It is found in Japan, China, and Philippines, etc.
Symptoms
Patients infected with S. haematobium suffer from terminal haematuria and
Symptoms
Patients infected with S. haematobium suffer from terminal haematuria and
during the incubation period: local cercarial dermatitis (swimmer’s itch) or general anaphylactic or toxic symptoms – fever, headache, malaise, and urticaria. This is accompanied by leucocytosis, eosinophilia, enlarged tender liver, and a palpable spleen;
during oviposition painless terminal hematuria (endemic hematuria), frequency of micturition and burning, hyperplasia and inflammation of bladder mucosa, with minute papular or vesicular lesions;
during tissue proliferation and repair: In the chronic stage, there is generalized hyperplasia and fibrosis of the vesical mucosa with a granular appearance (sandy patch). At the sites of deposition of the eggs, dense infiltration with lymphocytes, plasma cells, and eosinophils leads to pseudoabscesses. The entire mucosa becomes inflamed, thickened, and ulcerated. Secondary bacterial infection leads to chronic cystitis.
Chronic schistosomiasis has been associated with squamous cell carcinoma of the bladder.
Diagnosis
S. mansoni:
♦ Microscopic examination of the stool for eggs after concentration
Diagnosis
S. mansoni:
♦ Microscopic examination of the stool for eggs after concentration
♦ Rectal snip
S. haematobium:
♦ Urine Microscopy. Examination of the urine after allowing it to sediment in a conical urinalysis glass. A drop from the sediment is taken and examined for eggs. Egg has terminal spine.
♦ Biopsy from bladder
♦ Detection of specific schistosome antigens in serum or urine.
♦ Serological tests
♦ Intradermal skin tests
♦ Imaging (X-ray, cytoscopy, Ultrasonography (USG), Intravenous pyelogram (IVP))
Treatment
Praziquantel: single oral dose of 40 mg/kg divided into two doses.
Treatment
Praziquantel: single oral dose of 40 mg/kg divided into two doses.
Metriphonate 7.5 mg/kg. weekly for 3weeks.
Prevention
1. Health education:
A. On use of clean latrines and safe water supply. Effective treatment of infected persons.
Avoid swimming, bathing, and washing in infected water.
B. Avoid urination and defecation in canals, avoid contact with canal water
2. Snail control:
A. Physical methods:
i. Periodic clearance of canals from vegetations.
ii. Manual removal of snails and their destruction.
B. Biological methods: Use of natural enemies to the snails such as Marisa.
C. Chemical methods: Molluscides are applied in the canals to kill the snails. e.g. Endod
2. LIVER FLUKES
2. LIVER FLUKES
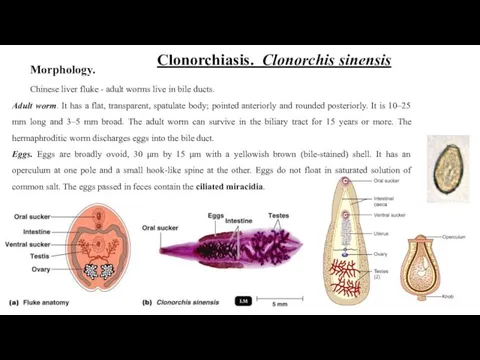
Clonorchiasis. Clonorchis sinensis
Morphology.
Chinese liver fluke - adult worms live in bile
Clonorchiasis. Clonorchis sinensis
Morphology.
Chinese liver fluke - adult worms live in bile
Adult worm. It has a flat, transparent, spatulate body; pointed anteriorly and rounded posteriorly. It is 10–25 mm long and 3–5 mm broad. The adult worm can survive in the biliary tract for 15 years or more. The hermaphroditic worm discharges eggs into the bile duct.
Eggs. Eggs are broadly ovoid, 30 μm by 15 μm with a yellowish brown (bile-stained) shell. It has an operculum at one pole and a small hook-like spine at the other. Eggs do not float in saturated solution of common salt. The eggs passed in feces contain the ciliated miracidia.
Symptoms:
The migration of the larva up the bile duct induces desquamation,
Symptoms:
The migration of the larva up the bile duct induces desquamation,
Patients in the early stage have fever, epigastric pain, diarrhea, and tender hepatomegaly. This is followed by biliary colic, jaundice, and progressive liver enlargement. Many infections are asymptomatic.
Chronic infection may result in calculus formation. A few cases go on to biliary cirrhosis and portal hypertension.
Some patients with chronic clonorchiasis tend to become biliary carriers of typhoid bacilli. Chronic infection has also been linked with cholangiocarcinoma.
Diagnosis:
The eggs may be demonstrated in feces (stool microscopy) or aspirated bile. They do not float in concentrated saline.
Several serological tests have been described including complement fixation and gel precipitation but extensive cross-reactions limit their utility. IHA with a saline extract of etherized worms has been reported to be sensitive and specific.
Intradermal allergic tests have also been described.
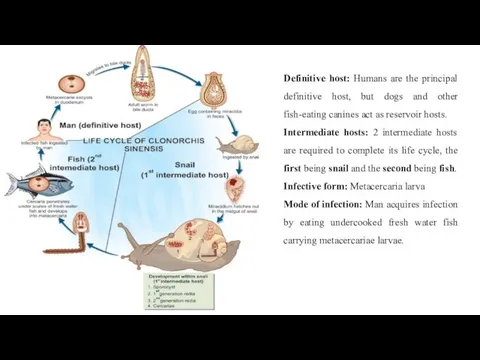
Definitive host: Humans are the principal definitive host, but dogs and
Definitive host: Humans are the principal definitive host, but dogs and
Intermediate hosts: 2 intermediate hosts are required to complete its life cycle, the first being snail and the second being fish.
Infective form: Metacercaria larva
Mode of infection: Man acquires infection by eating undercooked fresh water fish carrying metacercariae larvae.
Treatment:
Drug of choice is Praziquantel 25 mg/kg, 3 doses in
Treatment:
Drug of choice is Praziquantel 25 mg/kg, 3 doses in
Surgical intervention may become necessary in cases with obstructive jaundice.
Prophylaxis:
Proper cooking of fish
Proper disposal of feces
Control of snails.
Adults of Opisthorchis spp. are similar to, but often smaller than, Clonorchis sinensis. Adults
Adults of Opisthorchis spp. are similar to, but often smaller than, Clonorchis sinensis. Adults
Opisthorchiasis. Opisthorchis felineus
Definitive host: Humans are the principal definitive host, but dogs and other fish-eating canines act as reservoir hosts.
Intermediate hosts: 2 intermediate hosts are required to complete its life cycle, the first being snail and the second being fish.
Infective form: Metacercaria larva
Mode of infection: Man acquires infection by eating undercooked fresh water fish carrying metacercariae larvae.
Opisthorchis felineus is found mainly in Italy, Germany, Belarus, Russia, Kazakhstan, and Ukraine.
Diagnosis:
Microscopic identification of eggs in stool specimens.
The adult fluke can also
Diagnosis:
Microscopic identification of eggs in stool specimens.
The adult fluke can also
Serologic testing
Symptoms:
Most infections are asymptomatic. Most pathologic manifestations result from inflammation and intermittent obstruction of the biliary ducts. In mild cases, manifestations include dyspepsia, abdominal pain, diarrhea, or constipation. With infections of longer duration, the symptoms can be more severe, and hepatomegaly and malnutrition may be present. In rare cases, cholangitis, cholecystitis, and chlolangiocarcinoma may develop. In addition, fever, facial edema, lymphadenopathy, arthralgias, rash, and eosinophilia.
Diagnosis:
stool examinations
Imaging (ultrasound, CT, MRI).
Serologic testing
Treatment:
Praziquantel,
Diagnosis:
stool examinations
Imaging (ultrasound, CT, MRI).
Serologic testing
Treatment:
Praziquantel,
Albendazole, the dosage is 10mg/kg/day for 7 days. The pediatric dosage is the same. Albendazole should be taken with food; a fatty meal increases the bioavailability.
Prophylaxis:
Proper cooking of fish
Proper disposal of feces
Control of snails.
Fascioliasis. Fasciola hepatica
Morphology
Adult Worm. It is a large leaf-shaped fleshy fluke,
Fascioliasis. Fasciola hepatica
Morphology
Adult Worm. It is a large leaf-shaped fleshy fluke,
Egg. The eggs are large, ovoid, operculated, bile-stained, and about 140 μm by 80 μm in size. Eggs contain an immature larva, the miracidium. Eggs do not float in saturated solution of common salt. Eggs are unembryonated when freshly passed.
Symptoms:
In traversing the liver tissue, it causes parenchymal injury.
As humans are
Symptoms:
In traversing the liver tissue, it causes parenchymal injury.
As humans are
In acute phase during the migration of the larva, patients present with fever, right upper quadrant pain, eosinophilia, and tender hepatomegaly. The symptoms subside as parasites reach their final destination.
In chronic phase, patients may develop biliary obstruction, biliary cirrhosis, obstructive jaundice, cholelithiasis, and anemia. No association to hepatic malignancy has been ascribed to fascioliasis.
Occasionally, ingestion of raw liver of infected sheep results in a condition called halzoun (meaning suffocation).
The adult worms in the liver attach to the pharyngeal mucosa, causing edematous congestion of the pharynx and surrounding areas, leading to dyspnea, acute dysphagia, deafness, and rarely, asphyxiation.
Diagnosis:
Stool Microscopy
Blood Picture
Serodiagnosis
Imaging (USG, CT scan, Endoscopic Retrograde Choangiopancreatography (ERCP) and
Diagnosis:
Stool Microscopy
Blood Picture
Serodiagnosis
Imaging (USG, CT scan, Endoscopic Retrograde Choangiopancreatography (ERCP) and
Treatment:
triclabendazole (10 mg/kg once)
bithionol (30–50 mg for 10–15 days)
Prednisolone at a dose of 10–20 mg/kg is used to control toxemia.
Prophylaxis:
Health education
Preventing pollution of water courses with sheep, cattle, and human feces
Proper disinfection of watercresses and other water vegetations before consumption.
Life Cycle
F. hepatica passes its life cycle in 1 definitive host
Life Cycle
F. hepatica passes its life cycle in 1 definitive host
Definitive host: Sheep, goat, cattle, and man.
Intermediate host: Snails of the genus Lymnaea and Succinea. Encystment occurs on aquatic plants, which act as second intermediate host.
Mode of infection: The definitive host, sheep and man, get infection by ingestion of metacerceriae encysted on aquatic vegetation.

















 Болезни рыб. Диагностика и лечение
Болезни рыб. Диагностика и лечение Невропатология и дефектология
Невропатология и дефектология Situația epidemiologică privind infecția covid-19
Situația epidemiologică privind infecția covid-19 Науқастың жеке бас гигиенасы
Науқастың жеке бас гигиенасы Инфекции, передающиеся парентеральным путем (вирусные гепатиты В,С,Д, ВИЧ-инфекция)
Инфекции, передающиеся парентеральным путем (вирусные гепатиты В,С,Д, ВИЧ-инфекция) Қала және ауыл тұрғындары арасында. Созылмалы жүрек жеткіліксіздігі бар науқастардың
Қала және ауыл тұрғындары арасында. Созылмалы жүрек жеткіліксіздігі бар науқастардың Методики обогащения биологического материала(методы седиментации и флотации)
Методики обогащения биологического материала(методы седиментации и флотации) Сахарный диабет
Сахарный диабет Терінің вирусты аурулары
Терінің вирусты аурулары Аномалии конституции. Синдром внезапной смерти
Аномалии конституции. Синдром внезапной смерти Патофизиология клетки
Патофизиология клетки Туберкулез
Туберкулез Дуглас Дж. Ри Глаукома
Дуглас Дж. Ри Глаукома Аритмиялар
Аритмиялар Неотложные состояния при эндокринных заболеваниях (часть I)
Неотложные состояния при эндокринных заболеваниях (часть I) Строение и пластика черепа
Строение и пластика черепа Асқынған босану және кесар тілігі операциясынан кейінгі босанғаннан кейінгі кезеңді жүргізудің ерекшеліктері
Асқынған босану және кесар тілігі операциясынан кейінгі босанғаннан кейінгі кезеңді жүргізудің ерекшеліктері Bronchitis
Bronchitis Острая дыхательная недостаточность
Острая дыхательная недостаточность Дополнительные методы диагностики при черепно-мозговой травме. Показания к оперативному лечению
Дополнительные методы диагностики при черепно-мозговой травме. Показания к оперативному лечению Стресс. Виды стресса. Эмоциональный стресс. Клинические проявления стресса
Стресс. Виды стресса. Эмоциональный стресс. Клинические проявления стресса Эндокринная система
Эндокринная система Презентация 1
Презентация 1 Профилактика психических заболеваний
Профилактика психических заболеваний Миотония. Пароксизмальная миоплегия
Миотония. Пароксизмальная миоплегия Перефкрическая сенсо-моторная нейропатия у больных сахарным диабетом 2 типа
Перефкрическая сенсо-моторная нейропатия у больных сахарным диабетом 2 типа Внебольничная остановка сердца: комплекс кардиопульмональной реанимации на догоспитальном этапе у взрослого пациента
Внебольничная остановка сердца: комплекс кардиопульмональной реанимации на догоспитальном этапе у взрослого пациента Стратегические направления деятельности больницы
Стратегические направления деятельности больницы